
Transportation is a key accessibility issue for patients with HR-positive metastatic breast cancer receiving CDK4/6 inhibitors at community clinics.

Transportation is a key accessibility issue for patients with HR-positive metastatic breast cancer receiving CDK4/6 inhibitors at community clinics.

Findings from a real-world, head-to-head comparison show greater colorectal cancer risk reduction and safety with the use of a GLP-1RA vs aspirin.
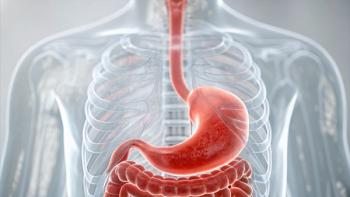
Median PFS over 1 year and median OS over 2 years have been observed for the first time in a phase 3 trial for gastroesophageal adenocarcinoma.

ECOG performance status of 1 was linked with worse patient-reported outcomes in patients with gastric or gastroesophageal junction adenocarcinoma.
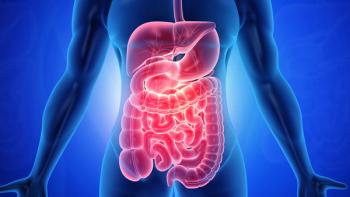
Zolbetuximab plus mFOLFOX6 and nivolumab led to meaningful gains in patients with unresectable gastric/gastroesophageal junction adenocarcinoma.
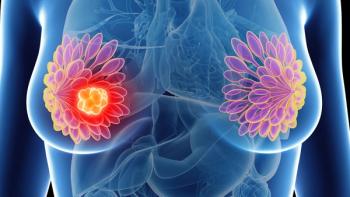
Destiny-Breast09 PROs demonstrated higher quality of life and fewer gastrointestinal symptoms in patients with HER2-positive advanced breast cancer.

Clinicians of color can experience higher rates of vicarious trauma when treating patients with cancer.

Nursing ethics expert Katherine Brown-Saltzman, MA, RN, shares insights on how to manage difficult ethical issues when treating patients with cancer.

Expert advice for administering and monitoring liso-cel in patients with follicular lymphoma.

The microbiota-based therapy MaaT013 showed promising efficacy and manageable safety in those with acute GVHD with gastrointestinal involvement.

Look back at the top 5 updates for oncology nurses and advanced practices providers published in 2025.

Patient K.C. transitions from high-risk care to invasive mammary carcinoma treatment under the care and support of a breast cancer advanced practice provider.

Age and having children were found to affect whether premenopausal women with breast cancer opted for fertility preservation.

Risvutatug rezetecan, an antibody-drug conjugate was granted FDA orphan drug designation for use in patients with small cell lung cancer.

Melinda Mayorga, RN, MSN, CNS, AGCNS-BC, OCN, discusses end-of-life care from a multidisciplinary perspective.

Oncology nurses and APPs are key players in patient education on precision medicine.

Subcutaneous mosunetuzumab wins FDA accelerated approval in patients with R/R follicular lymphoma following 2 or more lines of systemic therapy.

Breast cancer survivors improved cognitive outcomes with both real and sham acupuncture, but real acupuncture showed greater gains.

As CAR T-cell therapy expands to solid tumors, oncology nurses play a key role in monitoring, educating, and supporting patients.
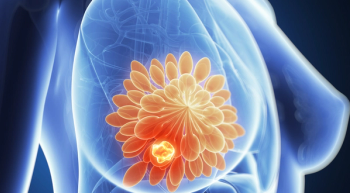
Giredestrant displayed a safety profile consistent with prior findings and had a lower rate of discontinuation compared with standard endocrine therapy.

Frontline maintenance tucatinib plus trastuzumab and pertuzumab increased progression-free survival in patient with HER2-positive metastatic breast cancer.

The FDA has approved the use of subcutaneous amivantamab and hyaluronidase-lpuj across all amivantamab indications.

The FDA has greenlit treatment with rucaparib for previously treated patients with BRCA-mutated metastatic castration-resistant prostate cancer.
A mobile health intervention was linked with an increase in general and cancer-specific QOL in adolescent and young adult breast cancer survivors.

Hormone replacement therapy was associated with a lower risk of developing BRCA1- or BRCA2-mutated breast cancer among those already at higher risk.

The treatment combination of T-DXd and pertuzumab was granted FDA approval in the first-line for unresectable or metastatic HER2-positive breast cancer.

The FDA has approved niraparib and abiraterone acetate with prednisone for the treatment of patients with BRCA2-mutated metastatic hormone-sensitive prostate cancer.
Subcutaneous daratumumab plus teclistamab improved survival outcomes in patients with R/R multiple myeloma vs standard daratumumab-based regimens.
Preoperative radiation and pembrolizumab improved T-cell infiltration in patients with higher-risk, HR-positive, HER2-negative, early-stage breast cancer.
Phase 2 data demonstrated similar pharmacokinetic profiles between subcutaneous azacitidine and an oral combination of azacitidine and cedazuridine.